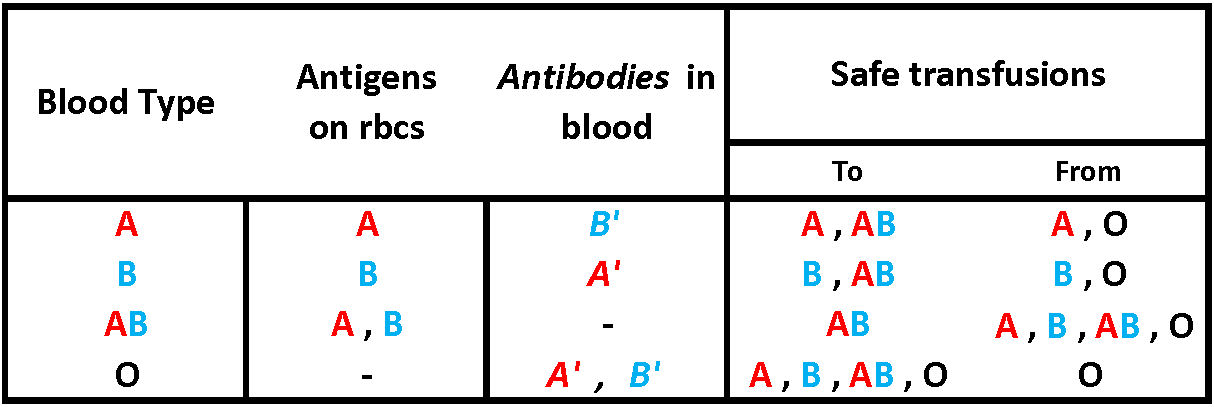
Co-dominant blood & antigen compatibility in the ABO blood group system

Blood-type in the ABO system is determined by three alleles (IA , IB , IO) at the Isoagglutinin locus on Chromosome 9. The IA and IB alleles determine antigenic proteins on the surface of red blood cells, which in turn cause the immune system to develop antibodies against the antigen not present. An individual who is IAIB has both antigens, and therefore does not generate antibodies to either: alleles IA and IB are thus co-dominant. Individuals who are IAIA or IAIO have the same blood type and generate anti-B antibodies: IA is thus dominant to IO. The same principles apply to IBIB and IBIO, such that IB is dominant to IO. An individual who is IOIO has no antigens, and generates antibodies to both.
The test for ABO blood type involves
mixing purified A' (anti-A) and B' (anti-B) antibodies with the blood
to be typed. Type A
blood coagulates in the presence of A' antibody only, type B reacts with B'
antigen only, type AB with
neither, and type O with
both. The same reaction would occur in vivo, which necessitates typing of blood
prior to transfusion. Persons with an IA or IB allele cannot receive blood from a person
with either an IB or an IA allele, respectively. That is, type A persons cannot receive
Type B or AB blood, and vice versa.
In TV medical
shows, the frequent request for "O negative" blood reflects the
fact that Type O blood
is compatible with any ABO blood
type: Type O is thus
described as the 'universal donor'. Type AB is a 'universal
recipient' due to the lack of antibody production,
which is fortunate because the AB type is the rarest.
"Negative" refers to the second major blood-type locus, the Rh (Rhesus ) factor, with two alleles Rh+ and Rh-, where the first is a simple dominant to the second and produces an antigen absent in the second. Following the same principles as in ABO, Rh- blood can be safely transfused to any recipient. Note that Rh- persons constitute only ~15% of the North American population.
| Country | O+ | A+ | B+ | AB+ | O- | A- | B- | AB- | |
|---|---|---|---|---|---|---|---|---|---|
| Canada | 39.0% |
36.0% |
7.6% |
2.5% |
7.0% |
6.0% |
1.4% |
0.5% |
| United States | 37.4% | 35.7% | 8.5% | 3.4% | 6.6% | 6.3% | 1.5% | 0.6% |
|---|